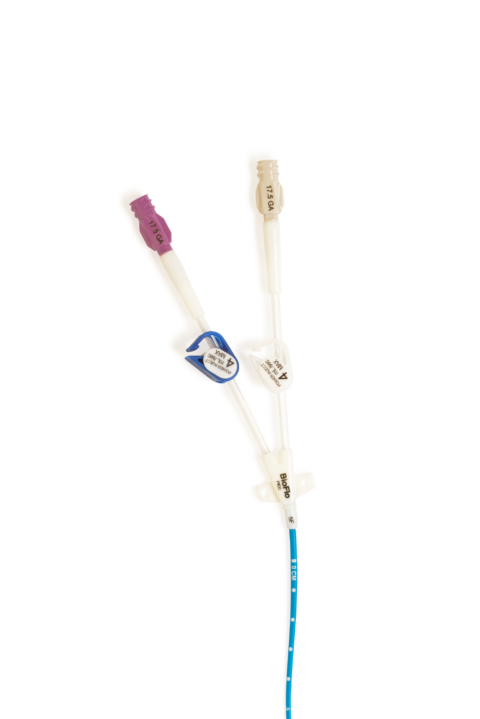
PICC-line care:
How to stay safe and comfortable
Peripherally inserted central catheters (PICC in short) have become increasingly common in medical practice. They provide a reliable access to administer medication, fluids, nutrition, or blood products directly into the bloodstream. This proves particularly valuable when patients require intravenous treatment for an extended period, ranging from several weeks to months. A PICC line offers significant benefits – but only with careful maintenance and strict adherence to hygiene protocols. Otherwise, patients might suffer from complications such as infection, blockage, or dislodgement. This article offers detailed, evidence-based guidance for PICC-line care. It is intended for patients and caregivers who deal with central-venous access devices on a day-to-day basis.
Overview
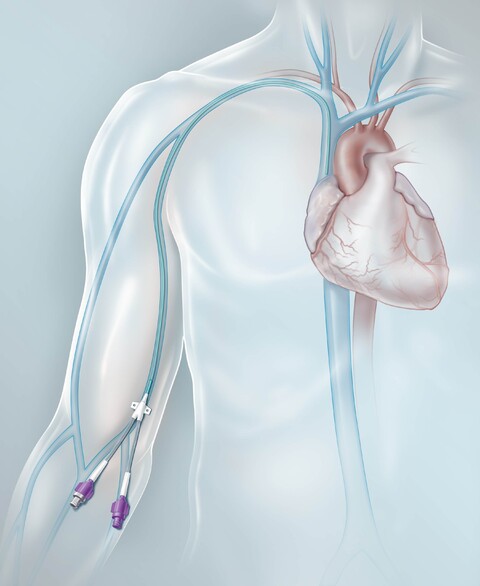
A PICC is a long, thin, flexible tube inserted into a vein in the upper arm – typically the basilic, cephalic, or brachial vein. From there, the catheter leads to a large central vein near the heart, typically the superior vena cava. Thanks to its positioning, the line provides access to a major blood vessel with strong and rapid flow. This allows for the administration of medication that might otherwise irritate or damage smaller peripheral veins.
The external portion of the PICC line normally includes one or more lumens (channels), depending on the patient’s needs. These lumens are colour-coded or labelled to distinguish their purposes. A single-lumen PICC may serve for one type of therapy, while a double- or triple-lumen PICC enables complex treatments (e.g. simultaneous administration of incompatible medications or drawing blood during ongoing infusions).
PICC-line placement
The initial insertion usually happens in a hospital, outpatient clinic, or specialised infusion centre. The patient receives local anaesthesia to numb the entry site, while ultrasound monitoring ensures accurate placement. Immediately after the insertion, the site is cleaned, secured with an adhesive stabilisation device, and covered with a sterile, transparent dressing.
Toolkit for PICC-line care
After the insertion procedure, patients will be provided with the supplies necessary to handle and protect their venous access. These include:
- alcohol-based hand sanitiser
- disposable drape
- alcohol pads
- disinfection caps
- needleless connectors
- dressings
- fixation device
- waterproof PICC covers
In addition, patients should also have a list of emergency numbers from their healthcare team that enables them to seek immediate help if needed.
PICC lines can be considered for any patient who requires a durable, long-term venous access. This includes people undergoing chemotherapy, prolonged antibiotic or antifungal therapy, or total parenteral nutrition (PN). The line can also be used for frequent blood sampling or repeated intravenous hydration, which means less discomfort caused by frequent needle sticks.
- Cancer patients often carry PICC lines, since these catheters allow for continuous or repeated infusions of drugs that might otherwise damage smaller veins.
- Patients with chronic infections such as endocarditis, osteomyelitis, or abscesses often benefit from PICCs as well because they enable convenient administration of antibiotics over several weeks. (This is called outpatient parenteral antibiotic therapy, short OPAT.)
- Individuals with gastrointestinal disorders that prevent nutrient absorption – e.g. Crohn’s disease, short bowel syndrome, or bowel obstruction – may become dependent on parenteral nutrition. This also requires permanent access to a large central vein to avoid irritation and ensure proper nutrient delivery, which can be provided through a PICC line.
- In some cases, PICCs are used for critically ill patients who need frequent laboratory draws or multiple IV medications.
- They might also come in handy for people with poor peripheral veins (due to older age, extensive scarring, or previous IV therapy). As the catheter can remain in place for a long period, it ensures continuous care and reduces the need for repeated insertions. In short: More safety and comfort for the patient.
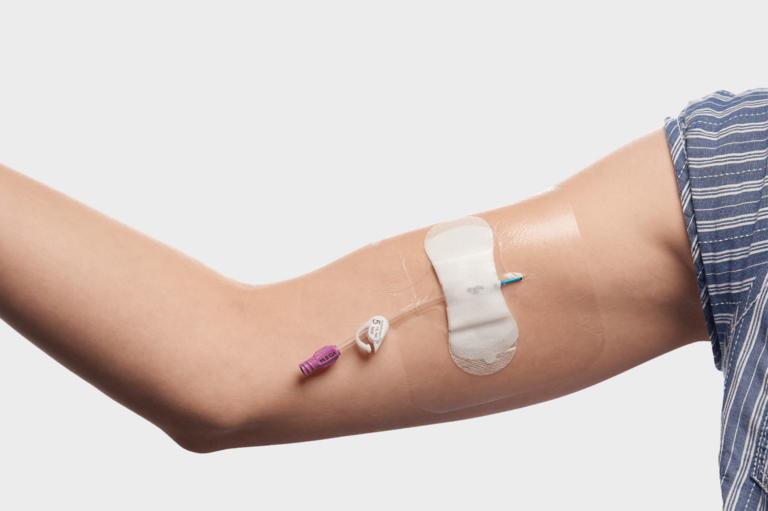
Patients and professionals may prefer PICC lines over other vascular-access devices (i.e. peripheral IVs, tunnelled central lines, or implanted ports) for several reasons.
- The most obvious advantage: Minimal discomfort. Since a PICC remains in place after its insertion, patients don’t have to go through the repeated needle sticks necessary for short-term IV lines.
- Another important factor: Safe access for administering potent or irritating medications. Drugs such as chemotherapy agents, concentrated electrolytes, or certain antibiotics can damage small peripheral veins. By delivering these substances directly into a large central vein, the PICC line dilutes them rapidly in the bloodstream. This reduces the risk of vein irritation or chemical phlebitis.
- PICC lines are versatile and durable, enabling multiple therapies simultaneously through separate lumens. They can be used for infusions, blood draws, or parenteral nutrition, remaining in place for several weeks or even months with proper maintenance.
- Compared to surgically inserted catheters or ports, PICC lines are relatively easy to place and remove. It usually requires only local anaesthesia and minimal recovery time.
- From a patient’s perspective, PICC-line care comes with more flexibility and independence compared to other venous-access devices. Many treatments can thus continue at home. This outpatient approach reduces hospital stays, improves quality of life, and often lowers healthcare costs.
Despite their benefits, central-venous access devices can cause certain complications.
- The most dangerous risk is an infection. Bacteria can enter the line during the insertion, dressing changes, or due to negligence of the proper aseptic technique. This may lead to an infection of the exit site or a catheter-related bloodstream infection (CRBSI). In the worst-case scenario, the latter might escalate into a life-threatening sepsis.
- Patients must also be careful to avoid thrombosis, the formation of blood clots around the catheter. This can cause swelling, pain, or discoloration of the arm or neck near the exit site. In some cases, blood clots can travel to the lungs and lead to a pulmonary embolism.
- Another common issue: Occlusion, i.e. blockage of the catheter. This can result from medication precipitates, blood clots, or kinking of the tubing. An occluded line may not be flush properly or allow blood to be drawn. Forceful flushing can damage the catheter or dislodge clots.
- Mechanical problems such as catheter dislodgement, breakage, or migration can occur if the line is accidentally pulled or not properly secured. If the catheter’s external part appears longer or shorter than usual, or if it leaks fluid, a medical professional should inspect it immediately.
Prevention is better than cure, no matter the type of complications. With proper PICC-line care and consistent monitoring, patients can minimise the chances of ever experiencing flow problems or developing an infection. Expert guidelines recommend following the aseptic non-touching technique (ANTT). This technique incorporates essential control measures to ensure that pathogenic microorganisms will not contaminate the venous-access device.
- ANTT starts with hand hygiene. Before handling a PICC line, everyone (including nurses, caregivers, and patients) must wash their hands thoroughly with soap and water and apply alcohol-based hand sanitiser. All manipulations of the line (e.g. connecting the tubing or flushing) should follow an aseptic, non-touch technique.
- Dressing maintenance also plays a crucial role for PICC-line care. The insertion site must be covered with a sterile, transparent, semipermeable dressing that makes it possible to inspect the site while protecting it against contamination. The dressing should be changed at least every seven days – sooner if it becomes damp, loose, or visibly soiled. During dressing changes, the skin should be cleaned using a 2 % chlorhexidine solution in 70 % alcohol.
- To avoid catheter dislodgement, the line should be secured with an appropriate stabilisation device such as a StatLock® or SecurAcath®. Adhesive tapes alone cannot sufficiently protect the catheter. The PICC’s external length should be measured and documented during each dressing change. Any alteration in length may indicate that the catheter has shifted position.
- Flushing and locking has proven highly effective in preventing blockages and infections. For flushing, we recommend the push-pause technique with saline: Intermittent flushing with 10 bolus doses of 1 ml each and a time interval of 0.4 seconds between two bolus doses. This creates turbulence within the catheter to dislodge small clots or residues. After flushing, a final positive pressure should be maintained. Needleless connectors (end caps) should be replaced at least weekly or whenever they become contaminated.
Lock solutions for PICC lines
Without antimicrobial protection, all sorts of germs will quickly find their way into the catheter. This leads to the formation of biofilm, consisting of microorganisms and a layer produced by those organisms that shields them against external influences. The longer pathogens linger there, the more they will become resistant to defence mechanisms of the immune system or antibiotics. In order to prevent catheter-related infections, we must therefore prevent the formation of biofilm in the first place. This is where a lock solution comes into play: It literally “locks” the line during the time periods in-between treatment sessions to protect it against the colonisation with microbes. To that end, TauroLock™ solutions contain taurolidine, an antimicrobial agent that kills more than 500 bacteria and fungi.
Depending on the patient’s disposition, there are different product variants with additional active ingredients. All variants have been approved for central-venous catheters and ports, including PICC lines.
| Product | Ingredients | Recommended Fields of Application |
|---|---|---|
 |
|
|
 |
|
|
 |
|
|
 |
|
|
 |
|
|
Besides all measures described above, regular inspection plays a crucial role in PICC-line care. Patients and caregivers should check daily for redness, swelling, pain, warmth, or fluid leakage. Any fever, chills, or malaise should be reported promptly, as these symptoms may signal an infection. Nurses should assess the patency each time they use the catheter. If they encounter resistance during flushing, they should not force it – otherwise the material might suffer damage.
Dos & don’ts for PICC-line care at home
- Regularly flush and lock the catheter at least once a week.
- Keep a log of dressing and flush dates.
- Change the dressing at least once a week.
- Inspect the site daily for signs of infection or displacement.
- Do not pull or tug on the catheter.
- Use a special cover during showering/bathing to keep the exit site dry.
- Dispose of used supplies in a closed bin.
- Never use scissors on the catheter.
- Never reuse needles, syringes, or other supplies.
- If supplies fall on the floor, throw them away.
- Keep the catheter’s clamps open and use needlefree connectors.
- Protect the end caps with an alcohol cover.
- Avoid strenuous activities (e.g. lifting objects heavier than 5 kg).
- Make sure that pets won’t come near the catheter.
Living with a permanent catheter is no easy feat – but it is not impossible either. As long as patients take necessary precautions, they can continue most normal activities safely.
One of the most common concerns is showering and bathing. Patients are generally allowed to shower, provided they protect the catheter and dressing from water completely. There are special products designed specifically for that purpose: water-resistant covers and fully waterproof exit pockets. With the latter, patients can even go swimming (if their physician approves). After any activity in the water, the dressing should be inspected to ensure it remains secure and dry. If it becomes damp or loose, it should be replaced as soon as possible.

- Patients should avoid exposing the catheter to lotions, powders, or perfumes near the exit site.
- Exercise can continue in moderation, except for activities involving vigorous or repetitive arm movement – e.g. tennis, golf, or weightlifting. The affected arm should not bear heavy loads (more than 2–5 kg). Gentle stretching and normal daily use of the arm, however, help maintain circulation and prevent stiffness. If patients experience pain or pulling at the site, they should stop the activity immediately.
- During sleep, patients should avoid lying directly on the arm that contains the PICC line. The catheter tubing can be gently looped and secured with medical tape or a mesh sleeve to avoid accidental tugging during the night.
- Travelling is feasible – as long as you plan ahead. Patients must pack all necessary supplies, including sterile flushes, dressings, and waterproof covers. They should also carry contact information of their healthcare provider or homecare nurse at all times, in case an emergency happens while on the road.
When to seek medical help
The sooner you recognise a potential problem, the better you can prevent serious complications. Patients should always contact their healthcare team if they experience fever, chills, or feel generally unwell. All these symptoms may indicate a bloodstream infection. Other red flags include:
- swelling, redness, or discharge at the exit site
- pain in the shoulder or arm where the PICC is placed
- swelling of the arm, neck, or face
- inability to flush or draw blood through the line
- leakage of fluid around the site or from the tubing
- sudden shortness of breath and chest pain (possible signs of air embolism or blood clot)
If the line accidentally comes out or breaks, the open end should quickly be clamped or pinched closed with sterile gauze to prevent air entry. The patient should then seek out a medical professional right away.
Once a patient has completed their treatment, or if a severe complication occurs, the catheter will be taken out. Performed by a professional and under sterile conditions, the removal only takes a couple of minutes:
- A nurse or physician cleans the area around the exit site.
- They proceed to gently withdraw the line while applying pressure to prevent bleeding.
A sterile dressing then remains on the exit site for 24 to 48 hours to allow the small vein to seal. Patients should keep monitoring the area for signs of infection or persistent bleeding during the first few days after the removal.